No products in the basket.
The Caldicott Principles are UK rules for using patient information in health and social care. They guide doctors, nurses and care staff on how to handle private health data in a safe and proper way. They help keep patient details private while still allowing sharing when care needs it.
In a basic sense, they solve a simple problem. Patient information must stay private, but doctors still need key details to give safe and right treatment. This balance matters more today because most health records now sit in digital systems. Different health services also share data more often across teams. At the same time, cyber attacks and data leaks are rising. So, clear rules are not just useful. They hold real value.
In this guide, we will explain the 8 Caldicott Principles and how they work in healthcare. We will also cover the role of Caldicott Guardians, the link with GDPR and real examples from UK healthcare.

What Are the Caldicott Principles?
How Did the Caldicott Principles Begin?
The Caldicott Principles started in 1997. Dame Fiona Caldicott directed a UK review at that time. She was a British psychiatrist. Her aim focused on stopping unnecessary sharing of patient information.
At that time, health services often shared more patient data than needed. So, the review brought in clear rules to control this. Over time, these rules became a key part of NHS confidentiality and data protection practice.
How Have the Caldicott Principles Evolved?
The Caldicott Principles did not stay the same. A later review called Caldicott2 in 2013 updated the rules. It expanded the original set into eight clear principles.
This change came as healthcare changed. Digital records became normal in hospitals and clinics. Also, different health services started sharing data more often. So, the rules had to match modern healthcare needs.
Today, the Caldicott Principles shape safe information use in UK health and social care.
Who Must Follow the Caldicott Principles?
Here are the main services that must follow these rules.
- NHS organisations – All NHS hospitals, trusts and services must follow these rules when handling patient data.
- GP practices – GP surgeries must use these rules when storing, accessing or sharing patient records.
- Social care providers – Care homes and social workers must follow these rules when handling personal care information.
- Publicly funded health services – Any health service paid for by the government must protect patient data and use it in a safe and careful way.
- Health and care teams handling patient data – Any team working with patient information must follow these rules.
Why Are Caldicott Principles Important in Healthcare?
How Do They Protect Patient Confidentiality?
The Caldicott Principles protect patient privacy in healthcare. They stop staff from sharing medical details without a real reason. This keeps sensitive information safe and under control.
At the same time, they build trust between patients and health services. When patients trust the system, they share clear and honest health details. As a result, doctors can give better and safer care.
How Do They Support Safe Information Sharing?
These principles guide safe sharing of patient information. They do not stop sharing. Instead, they set clear rules so people use data in the right way.
At the same time, they allow sharing when it supports treatment, care planning or patient safety. They also stop the unnecessary sharing of private details. So, the right people get the right information at the right time.
With this balance, health teams work better together. Patients also get faster care and more joined-up treatment across different services.
How Do They Reduce Compliance and Data Breach Risks?
Here are the practical ways it helps in healthcare:
- Set clear rules for using patient data in healthcare
- Reduce misuse of private health information
- Lower the risk of data breaches in NHS systems
- Help control digital health records in a safe way
- Support protection against cyber attacks in healthcare
- Improve how health services manage and protect information
What Are the 8 Caldicott Principles? Explained With Examples
Principle 1: Justify the Purpose for Using Confidential Information
Every use of patient data must have a clear reason. Staff must always know why they need the information. They should not access it out of habit or curiosity.
Example: A doctor checks a record to treat a patient. That is correct use. Checking a record without a care reason is not.
Principle 2: Use Confidential Information Only When Necessary
Staff should use patient information only when they truly need it. If they can use anonymous data, they should choose that instead. This helps keep personal details safe.
Example: A hospital uses anonymous data for a report because patient names are not needed.
Principle 3: Use the Minimum Necessary Confidential Information
Only the smallest amount of data should be shared. This helps reduce risk and protect privacy.
Example: A nurse shares only the diagnosis with another team, not the full patient history.
Principle 4: Access to Confidential Information Should Be on a Strict Need-to-Know Basis
Only people who need the information for their job should see it. This keeps patient data more secure.
Example: A receptionist handles bookings but cannot view full medical notes. A doctor can access them when needed.
Principle 5: Everyone With Access Must Understand Their Responsibilities
Anyone who works with patient data must handle it with care. Even small mistakes can cause serious problems.
Example: A staff member checks details properly before sending patient information to avoid errors.
Principle 6: Comply With the Law
All patient data use must follow UK laws like UK GDPR and the Data Protection Act 2018. These laws set clear rules for the safe use of information.
Example: A clinic only shares patient records when the law allows it.
Principle 7: The Duty to Share Information Can Be as Important as the Duty to Protect Confidentiality
Sometimes sharing information is needed to keep a patient safe. In some cases, not sharing can cause harm.
Example: A hospital shares information with social services in a child safety case.
Principle 8: Inform Patients and Service Users How Their Information Is Used
Patients should clearly know how their data is used. This helps build trust and avoids confusion. It also gives patients more control over their personal data.
Example: A GP practice gives patients a simple notice that explains how their records are used and shared.
Caldicott Principles Examples in Practice
Let’s look at how the Caldicott Principles work in real healthcare life. This helps us understand good practice, common mistakes and daily use in the NHS and social care.
What Does Good Information Sharing Look Like?
Good sharing means the right people get the right information at the right time. This keeps patient care smooth and safe.
In hospital discharge, staff send key details to the GP. As a result, the patient continues care at home without any gaps. In GP referrals, doctors share only the medical details that matter for treatment. They do not send full records unless they are needed. In safeguarding cases, teams act fast and share key information to protect children or vulnerable adults. This helps keep people safe and reduces risk. In team care, doctors, nurses and social workers share updates. So, they can plan care together in a clear and safe way.
What Does Poor Information Sharing Look Like?
Poor sharing creates problems in two main ways. This affects patient safety and trust. Sometimes staff share too much information. As a result, private details get exposed that no one needs. This puts patient privacy at risk.
At other times, staff do not share enough. This can slow down treatment or affect patient safety. Common mistakes include sending full records when only small details are needed. It also includes holding back key information due to fear of breaking rules. Both situations harm patient care and reduce trust in health services.
How Are Caldicott Principles Used in Daily NHS Practice?
In daily NHS work, staff use these principles to make quick and safe decisions. They choose who can see patient information, what to share and how much detail is needed. Across hospitals, GP surgeries and social care, these rules guide everyday work. They keep actions clear and the same across all teams.
As a result, teams protect patient privacy. At the same time, they still deliver safe and joined-up care for patients.
What Is a Caldicott Guardian and Why Is the Role Important?
What Does a Caldicott Guardian Do?
A Caldicott Guardian is a senior leader in a health or care organisation. They look after how patient information is used and shared and step in when decisions are not clear or feel sensitive. Also, they guide staff to handle data in a safe and careful way.
People often call this role the “conscience of the organisation”. This means they help people choose the right action for patients, not just the easiest one.
What Are a Caldicott Guardian’s Responsibilities?
Here are the core tasks they follow in healthcare settings:
- Give advice when data sharing decisions are complex or unclear
- Support staff to follow UK GDPR rules and data protection policies
- Check risks before sharing sensitive patient information
- Help teams balance patient safety with privacy
- Improve safe practice in how organisations use and share data
Which Organisations Need a Caldicott Guardian?
Any organisation that handles private health or care information should have a Caldicott Guardian. This includes NHS trusts, GP practices, mental health services and integrated care bodies. In these places, a Caldicott Guardian helps keep patient information safe and supports proper data sharing.
National Data Guardian guidance also covers many publicly funded care providers outside the NHS. This includes care homes and some private providers. Sometimes, smaller organisations can share one Caldicott Guardian if needed.
The main idea is clear. If an organisation uses sensitive patient information, it needs the right oversight. That is where a Caldicott Guardian helps. They protect confidentiality and also make sure important information can be shared safely when needed.
What Is the National Data Guardian’s Role?
How Does the National Data Guardian Support Data Protection?
The National Data Guardian (NDG) helps people trust how health and care information is used. It speaks for patients and the public. It also gives clear advice on how organisations should keep confidential information safe. This advice helps health and care services make good choices about privacy, sharing information and handling data properly. As a result, patient information stays protected and is used in the right way.
How Does the National Data Guardian Work With Caldicott Guardians?
The National Data Guardian gives national guidance on using confidential information. Then Caldicott Guardians use that guidance in everyday work inside their organisations. Their jobs are different but they work together closely.
The NDG gives direction while Caldicott Guardians help put that guidance into practice. In this way, they support lawful and ethical use of information and help keep patient trust strong.
How Do Caldicott Principles Relate to GDPR?
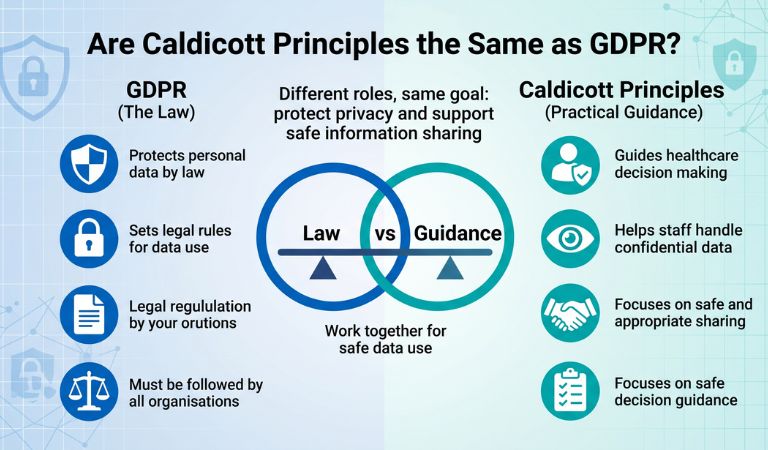
Are Caldicott Principles the Same as GDPR?
The Caldicott Principles and GDPR are not the same, but they work closely together. GDPR is the law that protects personal data. At the same time, the Caldicott Principles help health and care staff make the right decisions when using confidential information. One gives legal rules. The other gives practical guidance. In this way, they help protect privacy and support safe information sharing.
How Do They Work Together in Healthcare?
In healthcare, the Caldicott Principles and GDPR work toward the same goal. They both support data minimisation, which means only using information that is needed. They also support lawful processing, so patient data is handled in the right way. At the same time, they support confidentiality and accountability. As a result, organisations can keep private information safe and still share it when patient care needs it.
Common Misunderstandings About GDPR and Caldicott
Many people think GDPR stops information sharing, but that is a common myth. GDPR does not stop sharing when it supports patient care, keeps people safe or meets legal duties. In fact, it helps people share information in the right way.
Another misunderstanding is that consent is always needed before information can be shared. That is not always true in healthcare. At the same time, organisations can share information for other lawful reasons, especially when care or safeguarding is involved.
Some people can also become too careful and avoid sharing information when they should. This is called under-sharing. As a result, care may be delayed and patient risks can grow. This is where the Caldicott Principles help. They give clear guidance, so professionals can share information with confidence while still protecting privacy.
Best Practices for Applying Caldicott Principles
How Can Organisations Apply the Principles Effectively?
Key steps every team should follow:
- Check why you need to share the information
- Share only what is needed for the task
- Limit access to the right people only
- Train staff often, so they know what to do
- Review your data-sharing rules from time to time
When Should You Consult a Caldicott Guardian?
Sometimes, a decision may feel unclear or sensitive. In that case, it is best to ask for help. A Caldicott Guardian supports you in making safe and fair choices. You should speak to them when a request feels new or confusing. You should also ask when the risk is high or the case is sensitive. At the same time, if a safeguarding case becomes complex, their guidance can help you move forward with confidence.
5-Step Caldicott Compliance Checklist
Clear checks before any data goes out:
- Ask if sharing is really needed
- Choose only the exact details required
- Remove anything that is not needed
- Check who can access the information
- Write down the reason for sharing clearly
Do Caldicott Principles Apply After Death?
Yes, the Caldicott Principles apply to deceased patients too. Confidentiality does not end when a patient dies. Health records stay private and need care, respect and safe handling. Many people think these records become open after death, but that is not true.
Still, there are situations where sharing is allowed. Legal reasons may require it. Safeguarding concerns can also make it necessary. In some cases, public interest can support sharing too.
Even then, Caldicott Principles guide every decision. They help staff think before sharing any information. They make sure only the needed details are shared, nothing more. So the rule stays simple. Respect privacy first and share only when there is a clear and strong reason.
Conclusion: Why the Caldicott Principles Still Matter
The Caldicott Principles control how patient data is used, shared and stored safely. At the same time, They ensure information moves in a safe and limited way between teams. So, privacy stays protected and care decisions still move forward without delay. They also support legal and fair sharing where staff only use the information they truly need.
Today, healthcare uses more digital systems. So, data safety is more important than before. Even then, Caldicott Principles still guide daily work in every step. They help build trust between patients and health services. Strong information governance is not just about protecting data. It is also about using data in the right way to improve patient care.
Frequently Asked Questions (FAQs)
1. What are the 8 Caldicott principles?
- The 8 Caldicott Principles guide safe use of patient information in health care. They make sure staff only use and share data when needed and always protect privacy.
2. What are the 7 core principles of care?
- The 7 core principles of care focus on good, safe and kind support. They include dignity, respect, safety, teamwork, clear communication, quality care and person-centred support.
3. Does the Caldicott principle apply to information related to the deceased?
- Yes, the Caldicott Principles still apply after death. Patient records stay private and staff must handle them with care. Sharing only happens in special cases like legal needs, safety or public interest.
4. What are the 7 key principles of data protection?
- These principles make sure personal data stays safe and fair to use. They include lawful use, clear purpose, data minimisation, accuracy, storage limits and strong security.
5. What are the 7 personal data protection principles?
- These rules protect personal information from misuse. They focus on fair use, safe storage, correct data and using information only for the right reason.
6. What is the 7 clause of the GDPR?
- GDPR does not have a “7 clause” rule. It sets key principles that guide organisations to use and protect personal data safely and lawfully.
7. What are the 6 rules of GDPR?
- The 6 GDPR principles guide safe handling of data. They include lawful use, clear purpose, data minimisation, accuracy, storage limits, and strong protection.
8. What is the principle 7 of the Data Protection Act 1998?
- Principle 7 tells organisations to protect data with strong security. Organisations must protect personal data from loss, damage, or misuse using safe systems and controlled access.
